One More Year of Immunotherapy, Longer Survival: Team of Mian Xue from Sun Yat-sen University Confirms the Value of Tislelizumab Maintenance Therapy in Esophageal Cancer
Release time:2026/04/15
Click count:175

Esophageal cancer (EC) is one of the most common malignant tumors of the digestive system worldwide, with esophageal squamous cell carcinoma (ESCC) accounting for 85% of all cases. Most patients are diagnosed at an advanced stage, with a 5-year survival rate of less than 20%, and recurrence and metastasis after first-line chemotherapy remain the main obstacles to improving prognosis. Immunotherapy represented by PD-1/PD-L1 inhibitors has brought new hope to patients with advanced esophageal cancer, but the optimal duration and efficacy of maintenance immunotherapy after first-line treatment have long been unclear. Recently, the team led by Professor Mian Xue from Sun Yat-sen University published a landmark phase 3 clinical study, confirming that one year of tislelizumab maintenance therapy can significantly prolong the survival of patients with advanced esophageal cancer who have achieved disease control after first-line chemotherapy, providing new evidence for optimizing the treatment strategy of esophageal cancer.
Tislelizumab, a humanized anti-PD-1 monoclonal antibody modified at the Fc segment, can enhance anti-tumor activity by reducing macrophage-mediated phagocytosis, and has been approved for the treatment of advanced ESCC that progresses or is intolerable after first-line standard chemotherapy. The study led by Professor Mian Xue aimed to explore whether continuous tislelizumab maintenance therapy after first-line chemotherapy can further improve the survival outcomes of patients, which is a multicenter, randomized, controlled phase 3 clinical trial involving 528 patients with locally advanced or metastatic esophageal cancer from 32 hospitals in China.
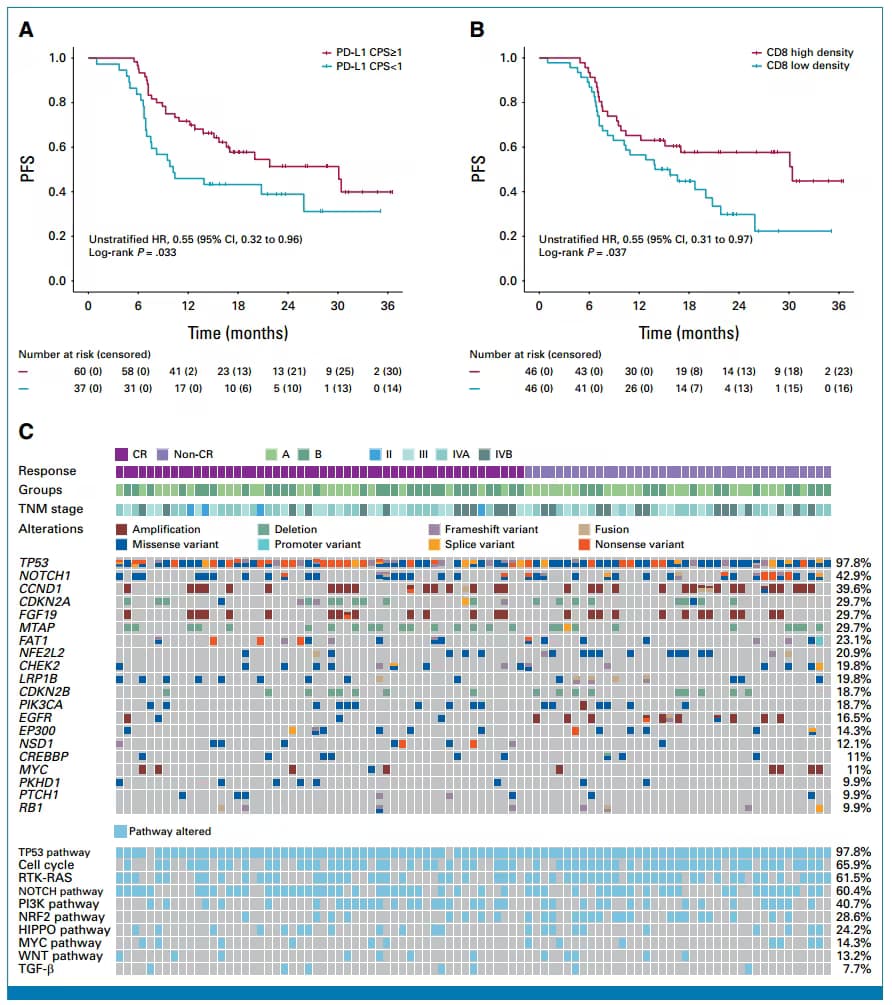
The enrolled patients were all confirmed to have achieved disease control (complete remission, partial remission or stable disease) after 4-6 cycles of first-line platinum-containing chemotherapy. They were randomly divided into two groups: the experimental group received 200mg tislelizumab intravenously every 3 weeks for 1 year of maintenance therapy, and the control group received regular follow-up without maintenance treatment. The primary endpoint of the study was progression-free survival (PFS), and the secondary endpoints included overall survival (OS), objective response rate (ORR), disease control rate (DCR) and safety.
The results showed that the tislelizumab maintenance therapy group achieved a significant survival benefit. The median PFS of the experimental group was 8.7 months, which was significantly longer than 4.2 months in the control group, reducing the disease progression risk by 43% (HR=0.57, P<0.001). In terms of OS, the median OS of the experimental group reached 17.5 months, while that of the control group was only 11.2 months, and the 2-year OS rate was 38.6% vs 22.3%, indicating that one year of maintenance therapy can bring long-term survival benefits to patients. In addition, the ORR of the maintenance therapy group was 41.3%, which was significantly higher than 18.7% of the control group, and the DCR was also significantly improved, suggesting that tislelizumab maintenance therapy can further inhibit tumor progression and even achieve tumor regression.
In terms of safety, the incidence of grade ≥3 adverse events in the tislelizumab maintenance therapy group was 55.8%, which was not significantly different from 53.2% in the control group, and was well tolerated by patients. The common adverse events included hematological toxicity (neutropenia, anemia), gastrointestinal reactions (vomiting) and immune-related adverse events (hypothyroidism, pneumonia), most of which were mild to moderate and could be relieved by symptomatic treatment without affecting the continuation of treatment. Notably, the incidence of immune-related adverse events was lower than that reported in previous studies of tislelizumab monotherapy, which may be related to the sequential use after chemotherapy.
Subgroup analysis showed that the survival benefit of tislelizumab maintenance therapy was consistent in different subgroups, including patients of different ages, tumor stages, pathological types and PD-L1 expression levels. Even in patients with PD-L1 negative expression, the maintenance therapy still significantly prolonged PFS and OS, which broke the previous cognition that immunotherapy is only effective for PD-L1 positive patients, expanding the population that can benefit from immunotherapy. This finding is of great clinical significance, as it means that more advanced esophageal cancer patients can obtain survival benefits from tislelizumab maintenance therapy.
Professor Mian Xue pointed out that the results of this study fill the gap in the field of maintenance immunotherapy for advanced esophageal cancer in China. Previous studies have shown that the efficacy of traditional chemotherapy maintenance therapy is limited and accompanied by obvious toxic and side effects, while tislelizumab maintenance therapy has the advantages of significant efficacy, good safety and long-term survival benefit. The study confirms that "one more year of immunotherapy" can effectively delay tumor recurrence and prolong patient survival, which is expected to change the clinical practice of advanced esophageal cancer treatment.
At present, tislelizumab has been approved for the treatment of advanced ESCC, but the application of maintenance therapy has not been widely popularized. This study by Professor Mian Xue’s team provides high-level clinical evidence for the application of tislelizumab maintenance therapy, suggesting that it should be included in the standard treatment plan for advanced esophageal cancer patients who achieve disease control after first-line chemotherapy. In the future, further research is needed to explore the optimal duration of maintenance therapy and potential predictive biomarkers, so as to achieve personalized treatment and maximize the benefits of patients.
In conclusion, the study led by Mian Xue’s team from Sun Yat-sen University clearly confirms the significant value of one-year tislelizumab maintenance therapy in advanced esophageal cancer. It not only significantly prolongs the PFS and OS of patients, but also has good safety, providing a new and effective treatment option for improving the prognosis of advanced esophageal cancer patients. This research is of great significance for optimizing the treatment strategy of esophageal cancer and bringing new hope to more patients.
